Heel Pain
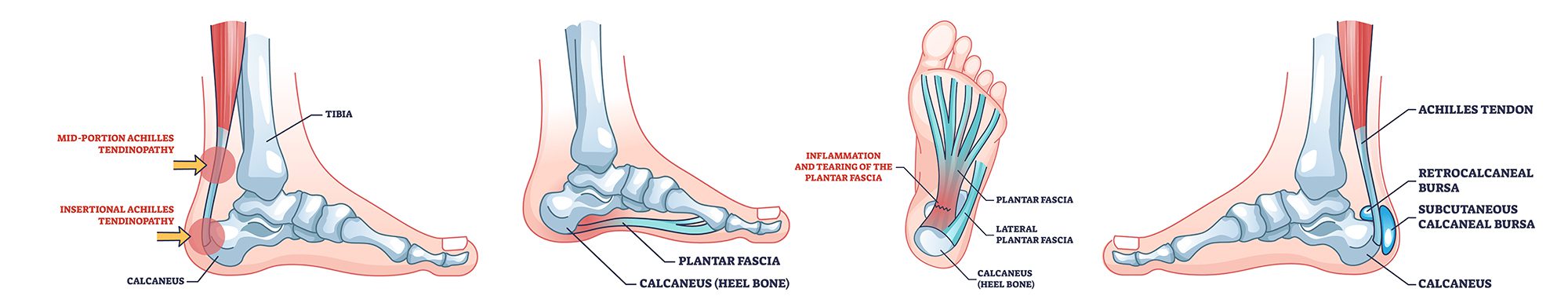
Table of Contents:
Heel Pain
Heel pain has many different causes. Plantar fasciopathy and Achilles tendon problems are by far the most common causes of heel pain. Heel pain however is also caused by:
- Acute injury
- Plantar lateral nerve impingement
- Tarsal tunnel syndrome
- Bursitis
- Plantar fat pad atrophy
- Stress fractures
- Growth plate injury or strain
- Lumbosacral radiculopathy (back pain)
- Bone or soft tissue tumors / growths
- Bone spurs
Plantar Fasciopathy (Fasciitis)
Plantar fasciitis is the most common cause of pain on the bottom (plantar side) of the heel. It is estimated 1 in 10 people will suffer from plantar fasciopathy at least once during their life. While it is commonly called plantar fasciitis, more accurate and better terminology would be plantar fasciopathy or plantar fasciosis.
- The “-itis” in plantar fasciitis refers to an inflammation of the fascia.
- Fasciosis is a degeneration of the fascia.
- Fasciopathy is a broader more encompassing term, indicating an abnormality or disorder of the fascia.
While acute inflammation and injury can occur, generally non-inflammatory thickening and degeneration of the plantar fascia are the problem. Heel spurs may be present, but rarely do they have any correlation to the presence of pain on the bottom of the heel. Plantar heel spurs are enthesophytes, a disorder of the plantar fascia’s attachment to the heel bone (calcaneus). Enthesophytes are caused by chronic degeneration and stress of the plantar fascia tissue at its attachment site on the periosteum of the heel bone.
The plantar fascia is a thick fibrous collagen band on the bottom of the foot connecting the heel to the forefoot. It helps support and stabilize the arch and facilitate shock absorption during gait. Pain is most often due to overuse. Overuse can be caused by changes in physical activity or exercise, exercise surface, and footwear.
Pain is most often due to overuse. Risk factors include:
• Increased physical activity on the foot, such as running, jumping, prolonged walking or standing.
• Wearing shoes which are worn out and no longer protect the foot.
• The weekend warrior, asymmetric activity distribution throughout the week or from week to week.
• Obesity
• Weight gain, such as with pregnancy, places extra stress and strain on the plantar fascia.
• Connective tissue disorders
• Age. Over time fascial tissue becomes less elastic and more susceptible to injury.
Common signs and symptoms of plantar fasciopathy are:
• Pain and stiffness on first weight bearing on the foot after rest or in the morning.
• Pain and stiffness during or after exercise or physical activity.
• Pain on the bottom of the heel or arch.
• Pain with activity.
• Limping.
• Swelling.
• Rest
• Activity modification
• Ice
• NSAIDs, such as ibuprofen (Motrin), naproxen (Alleve), or topical diclofenac (Voltaren, Flector)
• New supportive shoes. Regular replacement of shoes is recommended.
• Taping
• Arch supports or custom orthotics
• Stretching and foot strengthening exercises (check out the rehab page)
• Night splints. These are a good idea in theory and help passively stretch the lower leg. In reality however most people do not tolerate night splints well, finding them uncomfortable and difficult to sleep with.
• Cortisone injection
• Shockwave therapy (ESWT)
• Manual and physical therapy
• Immobilization
• Surgery
With the benefit of hindsight, prevention is the best treatment.
• Regularly replace shoes. How often shoes need to be replaced is dependent on activity level and the shoe itself. Most people do not replace shoes often enough.
• Use arch supports or custom orthotics
• Stretch and perform foot strengthening exercises (check out the rehab page)
• Avoid overuse. Gradually increase physical activity by no more than 10% per week.
Plantar fasciopathy is generally an overuse injury. Overuse leads to prolonged and excessive tension on the fascia.
Fortunately, surgery is generally not necessary. Over 90% of patients will get better without surgery. Surgery, when indicated, involves partial incision of the plantar fascia and possibly incision of the gastrocnemius fascia. Both of these procedures may be done with either an open incision or minimal incision endoscopic approach.
Plantar fasciopathy typically responds best when taking a wholistic multi-factorial approach and throwing the kitchen sink at it, rather than focusing on only one or two parts of the problem. Rest, ice, supportive shoes, and arch supports or custom orthotics are generally helpful. Rehab exercises for the foot and stretching exercises (check out the rehab page) are recommended. Steroid injections can be helpful when pain is significant.
Schedule an appointment now for an evaluation and discussion of your feet and their treatment options if:
• Pain and difficulty are not going away
• It is limiting physical activity
• It is affecting your quality of life
• Or you have questions
Call NOW for an Appointment:
Online Self- Scheduler:
Achilles Tendinopathy (Tendinitis)
Achilles tendinopathy is the most common cause of pain on the back (posterior side) of the heel and ankle. While it is commonly called Achilles tendinitis, more accurate and better terminology would be Achilles tendinopathy.
- The “-itis” in Achilles tendinitis refers to an acute inflammation of the tendon.
- Tendinosis is a more chronic degeneration of the tendon.
- Tendinopathy is a broader term indicating an abnormality or disorder of the tendon.
Achilles tendon injuries can be acute injures with inflammation, tears (rupture), or more chronic conditions with thickening and degeneration, longitudinal tearing of the tendon, calcifications, bursitis, enthesophytes, bone spurs, and prominence. Pain can be within the tendon itself or at its attachment onto the heel bone (calcaneus). In the absence of acute injury Achilles tendon injuries are most often due to overuse. Overuse can be caused by changes in physical activity or exercise, exercise surface, and footwear. Tendon and collagen tissue become less elastic as we age. This increases the risk of injury (tearing, rupture, and degeneration), particularly for weekend warriors or athletes who increase physical activity (faster, further, longer) without a gradual buildup.
The Achilles tendon is the largest (thickest) and strongest tendon in the body. It attaches the calf muscles to the heel bone (calcaneus). It is the largest and strongest tendon in the body due the heavy workload it shoulders. The Achilles tendon is subjected to tensile loading up to 10 times your body weight during dynamic physical activities such as running and jumping.
The Achilles tendon is named after the single area of weakness the otherwise invulnerable Greek hero Achilles had. The back of the heel, the Achilles tendon, is where the Greek warrior Paris fatally wounded Achilles with an arrow. Because of this story, one’s Achilles heel has become commonly associated with a fatal or catastrophic weakness in an otherwise strong and impervious system. Achilles was reportedly dipped into the river Styx as any infant by his mother Thetis. She held him suspended in the river by his left heel, leaving the heel untouched by the water, and vulnerable to injury. The legendary nature of this story shows signs of internal inconsistency as the story developed over time:
• The famous baptism in the river the Styx of Achilles by his mother is only found in later Roman sources rather than the earlier Greek traditions.
• It is unclear why the left heel was not dunked as well beneath the water.
• Before his death when Paris shot him in the left heel, the one spot not rendered invulnerable by the river Styx, Homer’s Iliad tells of Achilles being wounded on his elbow by Asteropaios, which does not fit very well with generalized invulnerability.
While an injury to the Achilles tendon can be painful and problematic, it would not be fatal, unless:
• Infection and sepsis occurred from an open wound created with a non-sterile object, such as an arrow.
• A poisoned weapon is used and no antidote is available.
• The posterior tibial artery in the ankle is also ruptured, which could result in significant blood loss.
• A blood clot occurs and migrates to the lungs, causing a pulmonary embolism.
• One is engaged in vigorous hand to hand combat to the death where sudden weakness to the ankle could be incapacitating and in turn fatal.
All of these scenarios are highly unlikely, meaning an injury to the Achilles tendon need not be your Achilles heel and lead to your ultimate downfall.
Pain can be due to overuse or acute injury. Risk factors include:
• Increased physical activity on the foot, such as running, jumping, prolonged walking or standing.
• Wearing shoes which are worn out and no longer protect the foot
• The weekend warrior, asymmetric activity distribution
• Connective tissue disorders
• Age. Over time fascial tissue becomes less elastic and more susceptible to injury.
• Obesity
• Weight gain, such as with pregnancy, places extra stress and strain on the plantar fascia
• Fluroquinolones. The use of some antibiotics (ciprofloxacin / Cipro, levofloxacin / Levaquin, moxifloxacin / Avelox, ofloxacin / Floxin) has been statistically associated with tendon injury and rupture during or up to three months after treatment, particularly in those greater than 60 years old.
• Injections in the tendon
Common signs and symptoms of Achilles tendinopathy are:
• Pain and stiffness during or after exercise or physical activity
• Pain and stiffness on first weight bearing on the foot after rest or in the morning.
• Pain on the back, or posterior side, of the heel / ankle
• Localized swelling or nodule formation to the tendon
• Bony enlargement on the back of the heel
• Localized redness
• Limping
• Weakness
• Swelling
• Rest and activity modification
• Ice
• NSAIDs, such as ibuprofen (Motrin), naproxen (Alleve), or topical diclofenac (Voltaren, Flector)
• New supportive shoes
• Taping
• Heel lifts
• Heel cushions / pads
• Arch supports or custom orthotics
• Stretching and foot strengthening exercises (check out the rehab page)
• Night splints – these are a good idea in theory and passively stretch the lower leg, but in reality most people do not tolerate them well and are not able to sleep with them.
• Shockwave therapy (ESWT)
• Manual and physical therapy
• Immobilization
• Steroid therapy with immobilization
• Surgery
With the benefit of hindsight, prevention is the best treatment.
• Regularly replace shoes. How often shoes need to be replaced is dependent on activity level and the shoe itself. Most people do not replace shoes often enough.
• Use arch supports or custom orthotics custom orthotics.
• Stretch and perform foot and ankle strengthening exercises (check out the rehab page).
• Avoid overuse. Gradually increase physical activity by no more than 10% per week.
Achilles tendinopathy typically responds best when taking a wholistic multi-factorial approach and throwing the kitchen sink at it, rather than focusing on only one or two parts of the problem. Rest, ice, supportive shoes, and arch supports or custom orthotics are generally helpful, with heel lifts. Rehab exercises for the foot and stretching exercises (check out the rehab page) are recommended.
Schedule an appointment now for an evaluation and discussion of your feet and their treatment options if:
• Pain and difficulty are not going away
• It is limiting physical activity
• It is affecting your quality of life
• Or you have questions
Call NOW for an Appointment:



